Blogs
- All
- Cardiac Sciences
- Clinical Psychology
- Critical Care
- Dentistry
- Dermatology & Cosmetology
- Emergency Medicine
- Endocrinology
- ENT, Neck & Head Surgery
- Gastro Sciences
- General Surgery
- Internal Medicine
- Neuro Sciences
- Obstetrics & Gynaecology
- Onco Care
- Ophthalmology
- Orthopaedics
- Paediatrics
- Plastic Surgery
- Psychiatry
- Pulmonology
- Renal Sciences
- Emergency
- Urology
- Liver Transplant & GI Surgery
- Dietetics & Nutrition
- General
Dermatology & Cosmetology
| Post Date : Apr 27, 2026
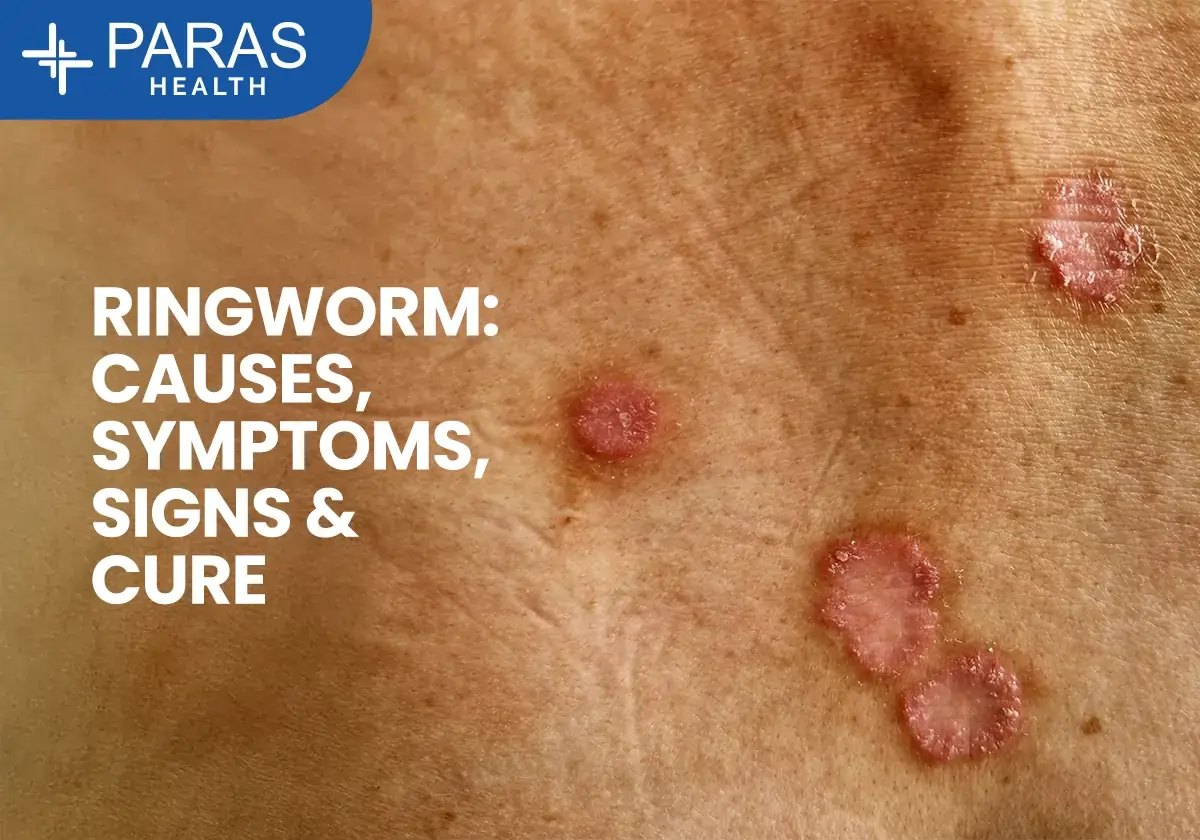
Ringworm infection is one of the most common fungal infections of the skin, yet it often creates confusion because of its name. Despite being called “ringworm,” it has nothing to do with worms. Instead, it’s caused by a group of fungi that thrive on the skin, scalp, and nails.
Continue Reading
Dietetics & Nutrition
| Post Date : Apr 27, 2026
Vitamin A is one of those nutrients that your body quietly depends on every single day. From helping you see clearly at night to keeping your skin healthy and your immune system strong, the benefits of vitamin A are wide-ranging and essential.
Continue Reading
Obstetrics & Gynaecology
| Post Date : Apr 25, 2026
Missing or delayed periods can feel stressful—especially when you’re unsure why it’s happening or how to fix it. If you’ve been searching for “how to get periods immediately” or “what to do if periods are late,” you’re not alone. Many women experience occasional delays due to lifestyle, hormonal changes, or underlying health conditions.
Continue Reading
Dietetics & Nutrition
| Post Date : Apr 23, 2026
When it comes to healthy dry fruits for women, dried apricots (also known as dry apricots) are often underrated. These small, golden-orange fruits are packed with essential nutrients that support everything from iron levels and hormonal balance to glowing skin and better digestion.
Continue Reading
Dietetics & Nutrition
| Post Date : Apr 21, 2026
Apricots may look like a simple fruit, but they are packed with powerful nutrients that can make a big difference to your health. From improving your skin and digestion to supporting heart health and weight loss, the health benefits of apricots are truly impressive.
Continue Reading
Dietetics & Nutrition
| Post Date : Apr 17, 2026
Looking for a simple, affordable food that can improve your hydration, support weight loss, and give your skin a natural glow? The answer might already be sitting in your kitchen — cucumber.
Continue Reading